Early detection of lymph node metastases can shape treatment decisions and improve outcomes in high-risk skin cancer.
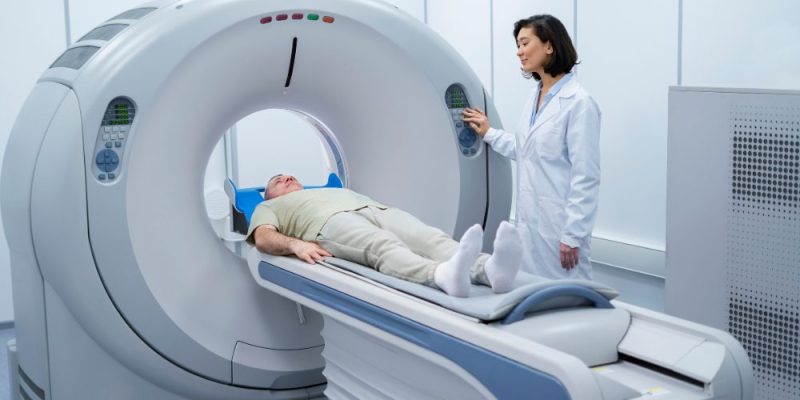
A recent multicenter study highlights a clear shift in how clinicians may approach diagnosis. Imaging tools such as ultrasonography and contrast-enhanced CT scans are proving far more effective than routine physical exams in identifying nodal spread, especially during initial staging.
This prospective diagnostic study took place across 13 tertiary dermato-oncology centers in Spain between January 2022 and April 2025. It included 155 patients diagnosed with high-risk cutaneous squamous cell carcinoma (cSCC). The average age was 80.3 years, and 21.9% of participants were women.
Each patient underwent three diagnostic methods within a defined perioperative window—one month before and after surgery:
1. Physical examination
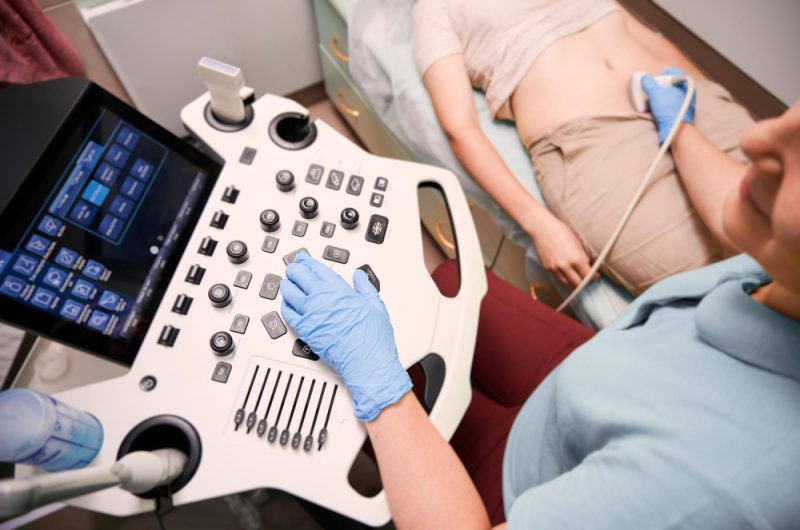
2. Ultrasonography
3. Contrast-enhanced CT
To confirm suspected metastases, clinicians used histopathologic analysis through fine-needle aspiration or lymph node excision. Patients with no initial signs of metastasis were monitored with a 3-month clinical follow-up.
Key Findings on Diagnostic Performance

Freepik | DC Studio | US and CT were far more sensitive than physical exams for detecting metastases.
The results reveal a strong advantage for imaging techniques over traditional exams. Ultrasonography achieved the highest sensitivity at 63.6%, followed by CT at 54.5%. In comparison, physical examination detected only 8.3% of nodal metastases.
Specificity remained high across all methods:
Ultrasonography: 95.6%
CT scans: 95.0%
Physical exam: 99.3%
Both imaging methods showed close agreement with each other, reflected by a Cohen kappa value of 0.87. Their diagnostic accuracy was also similar, with area under the curve (AUC) scores of 0.80 for ultrasonography and 0.75 for CT.
Physical exams showed weak agreement with imaging results, indicating limited reliability in detecting early nodal involvement.
Diagnostic accuracy varied significantly depending on patient immune status. In immunocompetent individuals, both ultrasonography and CT scans reached 100% sensitivity and delivered near-perfect accuracy (AUC 0.98). However, performance dropped sharply in immunosuppressed patients, with sensitivities falling to 20.0% for ultrasonography and 16.7% for CT.
Clinical Perspective and Expert Insight
Freepik | Drazen Zigic | High-risk cSCC staging should routinely include radiologic evaluation of lymphatic drainage.
The findings support routine use of imaging during baseline staging for high-risk cSCC. The study authors emphasized that radiologic evaluation of lymphatic drainage areas adds measurable value.
Selin Tokez, MD, PhD, and Marlies Wakkee, MD, PhD, from University Medical Center Rotterdam, noted that imaging “performs well in the detection of nodal metastasis, whereas clinical examination can fall short.”
They also pointed out that imaging plays an even greater role in high-risk groups. For immunosuppressed patients, regular surveillance imaging may help identify hidden metastases earlier and reduce the likelihood of extensive treatment complications.
Study Limitations to Consider
Despite strong findings, the study had limitations. The number of metastatic events remained relatively low, which may affect broader applicability. Variability in test timing, differences between centers, and operator-dependent factors also influenced results.
In addition, the study did not include routine short-interval follow-up imaging, which could have provided deeper insight into progression patterns.
Imaging techniques such as ultrasonography and contrast-enhanced CT offer a more reliable path for detecting lymph node metastases in high-risk cSCC compared to physical exams. While results are especially strong in immunocompetent patients, reduced sensitivity in immunosuppressed individuals signals the need for closer monitoring.
These findings reinforce the importance of incorporating imaging into standard staging protocols to support timely and accurate clinical decisions.